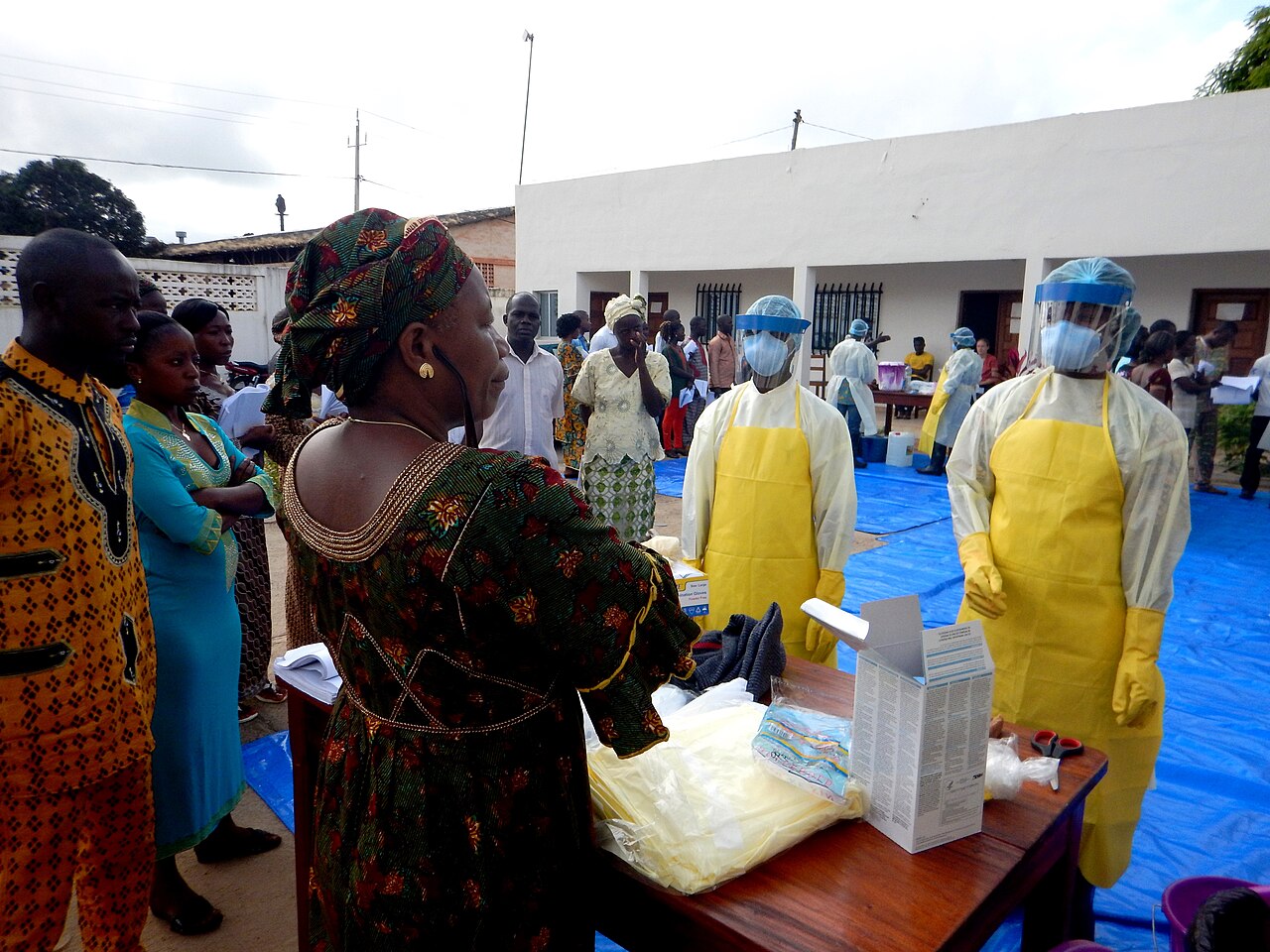
Ebola Virus Can Persist in Breast Milk Weeks After Recovery
New case study finds Ebola viral traces in breast milk 14 weeks post-recovery, raising urgent questions about infant feeding safety during outbreaks.
Overview
Ebola virus disease remains one of the most feared hemorrhagic fevers in the world — not only because of its severity during active infection, but because of the persistent questions surrounding what happens after a patient survives. A newly published case study has added a significant dimension to that picture: detectable traces of Ebola virus may remain present in breast milk for as long as 14 weeks after a survivor’s blood tests have returned negative, according to findings reported by the Center for Infectious Disease Research and Policy (CIDRAP).
This is not a report of a new outbreak. There are currently no declared Ebola emergencies at the scale of the 2014–2016 West Africa epidemic or the 2018–2020 Democratic Republic of Congo outbreak. Rather, this is a targeted clinical finding — a case study — that carries meaningful implications for how public health systems manage Ebola survivors, particularly breastfeeding mothers, during and after active outbreak responses.
The finding adds to a growing body of evidence that Ebola virus behaves in ways that conventional clearance testing may not fully capture. Blood-based PCR testing has long been the standard for declaring a survivor “recovered,” but viral persistence in so-called immunologically privileged sites — such as the eyes, testes, central nervous system, and now potentially breast milk — has complicated that picture considerably.
Current Situation
 Image: Wikimedia Commons
Image: Wikimedia Commons
The case study, published in late March 2026 and covered by CIDRAP, describes a single patient — a breastfeeding woman who survived Ebola virus disease and subsequently tested negative via blood PCR, the standard benchmark for recovery and discharge from care. Despite this negative blood result, viral material was detected in her breast milk at the 14-week mark post-recovery.
The precise viral load and whether the detected material constitutes replication-competent virus or residual genetic fragments are details that warrant further investigation. However, even the presence of viral RNA in breast milk at that duration is clinically significant. It raises the possibility, however small, that an infant fed by a survivor mother could be exposed to the pathogen at a point when the mother would conventionally be considered no longer infectious.
It is important to note the limitations of a single case study: findings from one patient cannot be generalized to all Ebola survivors without further research. Case studies are hypothesis-generating, not conclusive. That said, in the context of a virus with a case fatality rate historically ranging from 25% to 90% depending on the strain and access to care, even a potential transmission pathway deserves rigorous attention.
No confirmed infant infections linked to post-recovery breastfeeding have been attributed to this case, and the report does not indicate active transmission occurred. However, the implications for survivor care protocols are clear.
Affected Regions
 Image: Wikimedia Commons
Image: Wikimedia Commons
Ebola virus disease is endemic to sub-Saharan Africa, with the vast majority of outbreaks recorded in the Democratic Republic of Congo (DRC), Uganda, Guinea, Sierra Leone, and Liberia. The DRC alone has experienced more than a dozen separate Ebola outbreaks since the virus was first identified near the Ebola River in 1976.
The case study in question does not specify a country of origin for the patient, which limits geographic analysis. However, the public health relevance is inherently tied to the regions where Ebola outbreaks occur most frequently, where healthcare infrastructure may be strained, and where survivor follow-up programs — if they exist — operate under significant resource constraints.
Survivor populations in post-outbreak communities are often large in scale. Following the 2014–2016 West Africa outbreak, there were estimated to be more than 17,000 survivors across Guinea, Sierra Leone, and Liberia. Many of these individuals were women of reproductive age. The question of viral persistence in breast milk is therefore not a narrow clinical curiosity — it has population-level implications wherever outbreaks have occurred.
As of April 2026, no major active Ebola outbreak has been declared by the World Health Organization (WHO). The most recent outbreaks in the DRC were declared over in 2023. Surveillance continues in high-risk areas, and this new finding should be factored into both ongoing and future outbreak response planning.
Risk Assessment
The transmission dynamics of Ebola are well established: the virus spreads through direct contact with the blood, secretions, or bodily fluids of an infected or deceased person. Breast milk has long been recognized as a potential vehicle for transmission during active disease. What this case study forces us to reconsider is the duration of that risk window.
Survivors who test blood-negative may still carry Ebola virus in breast milk for months — meaning current clearance protocols based on blood PCR alone may be insufficient to protect breastfeeding infants.The WHO and other bodies have previously documented Ebola persistence in semen for up to 500 days post-recovery in male survivors, leading to extended sexual transmission risk windows and updated guidance on condom use. Breast milk has received considerably less systematic study as a persistence site, partly because fewer breastfeeding women have survived outbreaks to be enrolled in longitudinal studies. This case study underscores the need to correct that research gap.
Vulnerable populations most affected by this finding include:
- Infants born to or nursed by Ebola survivors, particularly in resource-limited settings where formula feeding may not be a safe or accessible alternative
- Healthcare workers who may handle breast milk from survivors in clinical or community settings
- Survivor support program staff who counsel women on post-recovery care
The broader public — those not in direct contact with survivors — faces no elevated risk from this finding. This is not a mechanism by which Ebola could spread in a generalized community setting.
Prevention & Response
Current WHO guidance for Ebola survivors includes counseling on potential viral persistence, sexual transmission risk reduction, and regular follow-up testing. However, specific, standardized guidance on breastfeeding cessation or breast milk testing timelines has not been uniformly codified across outbreak response frameworks.
This case study should prompt a review of those protocols. Several actionable steps are warranted at the institutional level:
Survivor follow-up programs operating in post-outbreak zones should incorporate breast milk screening alongside blood-based PCR testing for female survivors who are lactating. A negative blood result should not automatically be interpreted as whole-body clearance.
Infant feeding counseling for survivor mothers should be revisited. In settings where safe formula alternatives are available, the risk-benefit calculus for continued breastfeeding may shift following a positive breast milk test, even when blood tests are negative. This is a nuanced decision that must account for the well-documented risks of formula feeding in low-resource environments — including waterborne illness and malnutrition — against the potential, if unconfirmed, risk of viral transmission through breast milk.
Research investment into viral persistence across all bodily compartments in Ebola survivors remains urgently underfunded relative to the stakes. The scientific community currently lacks a comprehensive, longitudinal picture of how long various fluids may carry viral material in recovered individuals.
The WHO and national health ministries in Ebola-endemic regions should treat this finding as a signal requiring prospective study, not a confirmed transmission mechanism requiring immediate emergency response. The appropriate response is scientific rigor, not alarm.
For the general public and travelers, no change in behavior is indicated by this finding. Ebola does not spread through casual contact, respiratory droplets, or food and water. Risk is confined to direct exposure to bodily fluids of symptomatic or recently recovered individuals.
Sources
- CIDRAP (Center for Infectious Disease Research and Policy) — “Ebola virus may linger in breast milk for weeks after recovery,” March 30, 2026. https://www.cidrap.umn.edu/ebola/ebola-virus-may-linger-breast-milk-weeks-after-recovery
- World Health Organization — Ebola virus disease fact sheet and survivor care guidance. https://www.who.int/news-room/fact-sheets/detail/ebola-virus-disease