Avian Influenza Spreads Across Subtypes: H9N2 in Italy, H5N1 in Cambodia and US Poultry
Multiple avian flu subtypes are active globally: H9N2 imported to Italy from Senegal, H5N1 in Cambodia and US flocks, and H7 in Taiwan.
Overview
Avian influenza is rarely a single, tidy story. In recent weeks, at least three distinct subtypes of the virus have generated human or animal health alerts across four continents — a reminder that the global avian flu threat is not confined to any one strain or geography. The most striking new development is a confirmed human case of influenza A(H9N2) in Italy, linked to recent travel in West Africa, reported to the World Health Organization on 21 March 2026. Simultaneously, H5N1 has claimed a young child in Cambodia and continues to devastate commercial poultry in the United States, while H7 avian flu appeared in Taiwan with, according to authorities, no worrying mutations. Taken together, these developments underscore a period of heightened vigilance for pandemic preparedness planners, even as risk assessors stress that the immediate threat to the general public remains low.
Current Situation
 Image: Wikimedia Commons
Image: Wikimedia Commons
The Italian H9N2 case, confirmed through next-generation sequencing, involves an adult male who had recently returned from Senegal. The patient developed symptoms consistent with influenza, and Italian health authorities notified the WHO under the International Health Regulations (IHR 2005), which require mandatory reporting of any human infection caused by a novel influenza A subtype. Under those rules, the bar for notification is intentionally low: the mere novelty of the subtype — not the severity of the case — triggers reporting. Crucially, epidemiological investigation found no known history of exposure to live poultry and no contact with any individual displaying similar symptoms prior to illness onset, leaving the precise source of infection undetermined.
In Cambodia, a 3-year-old boy tested positive for H5N1 avian influenza, becoming that country’s third confirmed human H5N1 case of 2026, according to CIDRAP reporting from late March. Southeast Asia has long been an endemic hotspot for H5N1 in poultry, and Cambodia has recorded sporadic human spillover events for years, typically in children with direct poultry contact in rural settings.
In the United States, the scale of ongoing H5N1 activity in commercial and backyard poultry flocks remains substantial. According to CIDRAP, the US Department of Agriculture’s Animal and Plant Health Inspection Service (APHIS) confirmed outbreaks in 56 poultry flocks within a single 30-day window ending in early April, with Indiana among the hardest-hit states. No associated human cases from those flock outbreaks have been publicly confirmed.
In Taiwan, health officials reported a human case of H7 avian influenza in early April. Taiwanese authorities stated that genetic analysis of the virus showed no mutations that would be expected to increase the efficiency of transmission from birds to humans — a critical reassurance in any H7 detection, given that H7N9 caused significant human mortality in China between 2013 and 2017.
Affected Regions
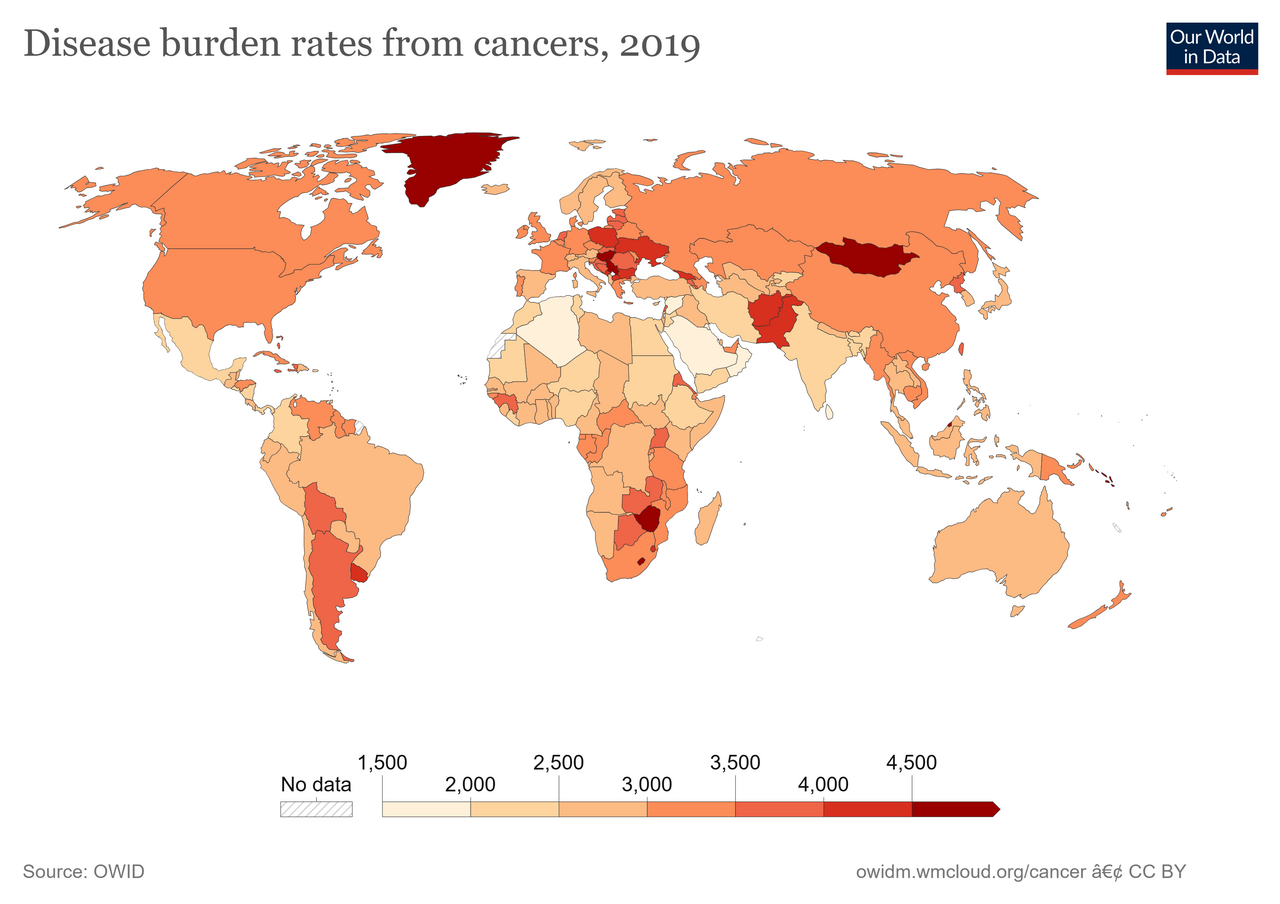 Image: Wikimedia Commons
Image: Wikimedia Commons
The geographic footprint of current avian influenza activity spans multiple WHO regions:
Europe: Italy has recorded what is described by the WHO as the first imported case of H9N2 linked to travel from West Africa — specifically Senegal. Italy itself is not known to have endemic H9N2 in its domestic poultry, making the West African exposure the presumed origin. European public health agencies have not indicated broader community exposure at this stage.
West Africa / Senegal: H9N2 is enzootic — meaning persistently present in animal populations — across parts of Asia and increasingly documented in African poultry. Senegal’s poultry sector, like much of sub-Saharan West Africa, faces ongoing challenges with avian influenza surveillance and biosecurity infrastructure. The Italian case raises questions about circulation of H9N2 among poultry or bird populations in Senegal that may be underdetected locally.
Southeast Asia: Cambodia remains a persistent hotspot for H5N1 human spillover. The country’s poultry-keeping culture, with live birds commonly kept in close proximity to households, creates repeated opportunities for zoonotic transmission, particularly among young children. Taiwan’s H7 detection adds another data point to a region with diverse avian influenza subtypes circulating in bird populations year-round.
North America: Indiana and surrounding states in the US Midwest represent the current epicenter of H5N1 activity in commercial poultry. The US outbreak, which has persisted across multiple production cycles, has already resulted in the culling of tens of millions of birds and has contributed to elevated egg and poultry prices. The density of commercial operations in the region makes containment challenging once a flock is affected.
Risk Assessment
For the general public in non-affected regions, including most of Europe and North America, the risk of acquiring avian influenza through routine daily activities remains very low — but travelers visiting areas with known poultry outbreaks should avoid direct contact with live birds, poultry markets, and surfaces contaminated with bird droppings.
The WHO classifies human infections caused by novel influenza A subtypes — including H9N2 — as events with “the potential for high public health impact,” which explains the mandatory IHR notification requirement. This classification is precautionary, not a declaration of elevated immediate risk. H9N2 has caused sporadic human infections globally for decades, predominantly in individuals with direct poultry exposure, and has not demonstrated sustained human-to-human transmission. The Italian case is notable precisely because the source of exposure remains unclear.
H5N1 carries a historically higher case fatality rate in humans — WHO data from prior years has placed it above 50% in confirmed cases globally, though this figure reflects severe cases more likely to be detected and reported, not the true infection fatality rate. Cambodia’s third pediatric case of 2026 fits a recognized pattern: young children with rural poultry exposure. Absent genetic changes that enhance human transmissibility, each case represents a contained spillover event rather than the beginning of sustained spread.
Vulnerable populations across all avian flu subtypes include individuals with direct or occupational poultry exposure — farm workers, live market vendors, veterinary personnel — as well as young children in endemic regions with household poultry. Immunocompromised individuals face heightened severity risk if infected.
The H7 detection in Taiwan carries its own historical weight, given the H7N9 epidemic that sickened approximately 1,500 people in China between 2013 and 2019. Taiwan’s rapid characterization of the virus and the finding of no concerning mutations is a model for the kind of transparent, timely genomic surveillance that allows risk to be accurately calibrated.
Prevention & Response
Italy has activated monitoring, contact tracing, and control measures consistent with IHR obligations following the H9N2 detection. The investigation into the patient’s travel history and possible animal exposures in Senegal is ongoing. Italian authorities have not indicated any secondary cases among contacts.
In the United States, APHIS continues to apply its standard response protocol to H5N1-affected flocks: mandatory depopulation of affected operations, movement restrictions in affected counties, and enhanced biosecurity guidance for producers. The scale of Indiana’s outbreak reflects both the density of the regional poultry industry and the persistent challenge of preventing viral introduction via wild bird migration corridors.
Cambodia has well-established protocols for H5N1 response developed over two decades of endemicity in the region. These include rapid case investigation, contact monitoring, and coordination with the WHO and the Food and Agriculture Organization (FAO). The country’s health ministry has historically been transparent in reporting, which helps maintain the integrity of global surveillance.
For travelers and the public, the WHO’s standing guidance on avian influenza prevention remains in effect: avoid direct contact with live poultry and wild birds; practice diligent hand hygiene, especially after visiting live animal markets; cook poultry and eggs thoroughly; and seek prompt medical evaluation if respiratory illness develops following potential exposure to birds or poultry environments.
No licensed human vaccine is currently in widespread use for any of the H9N2, H7, or H5N1 subtypes circulating in these events. Prepandemic candidate vaccines exist in national stockpiles for H5N1 and are being developed for H9N2 given its persistence as a candidate pandemic strain. The development of these stockpiles, and the rapid genomic surveillance exemplified by Taiwan’s response, represent the core pillars of the global preparedness architecture these events are stress-testing in real time.
Sources
- World Health Organization – Disease Outbreak News: Avian Influenza A(H9N2), Italy, 10 April 2026
- CIDRAP (Center for Infectious Disease Research and Policy) – Quick Takes: Human Avian Flu Case in Italy, 10 April 2026
- CIDRAP – Indiana Tracks More Avian Flu in Hard-Hit Counties, 9 April 2026
- CIDRAP – Quick Takes: H7 Flu Case in Taiwan, H5N1 Outbreaks in US Poultry, 2 April 2026
- CIDRAP – Quick Takes: H5N1 Avian Flu Case in Cambodia, 31 March 2026
Sources
- WHO Disease Outbreak News – Avian Influenza A(H9N2), Italy (DON597) ↗
- CIDRAP – Human Avian Flu Case in Italy, Salmonella Outbreak, New Polio Cases ↗
- CIDRAP – Indiana Tracks More Avian Flu in Hard-Hit Counties ↗
- CIDRAP – H7 Flu Case in Taiwan, H5N1 Outbreaks in US Poultry ↗
- CIDRAP – H5N1 Avian Flu Case in Cambodia ↗
